
The Knee Surgery Trap: New 10-Year Data Says Move, Don't Cut
A few years ago I had surgery to remove about 30% of my meniscus. I tried to deal with it without surgery first, and for a while I almost got away with it.
Here’s what that looked like. The knee would lock up — sometimes before class, sometimes mid-roll. A piece of cartilage would flip into the joint and I couldn’t straighten my leg. The first time it happened, a couple of guys in the morning crew helped me out. One pulled on my ankle while I shook the joint. The flipped piece popped back. After a minute of that, the knee felt good as new. I taught class that day.
That move — two training partners pulling on a locked knee in the middle of a gym — turns out to be a real, documented thing. There’s a 2025 case study from the American Osteopathic Academy of Orthopedics describing the same maneuver, done by a doctor, on the same kind of tear. So I kept doing it. Lock up, get help, pop it back, train.
The problem was that my tear was in the part of the meniscus that has no blood supply. No blood supply means no healing. Manual reduction kept working in the short run, but it couldn’t fix the underlying tear. The lock-ups got more frequent, not less. After a while, I gave up and had it done.
But here’s what I’ve learned since: most people who get told they need this surgery don’t actually need it. And the 2026 research is now embarrassingly clear about it.
The 10-year shock
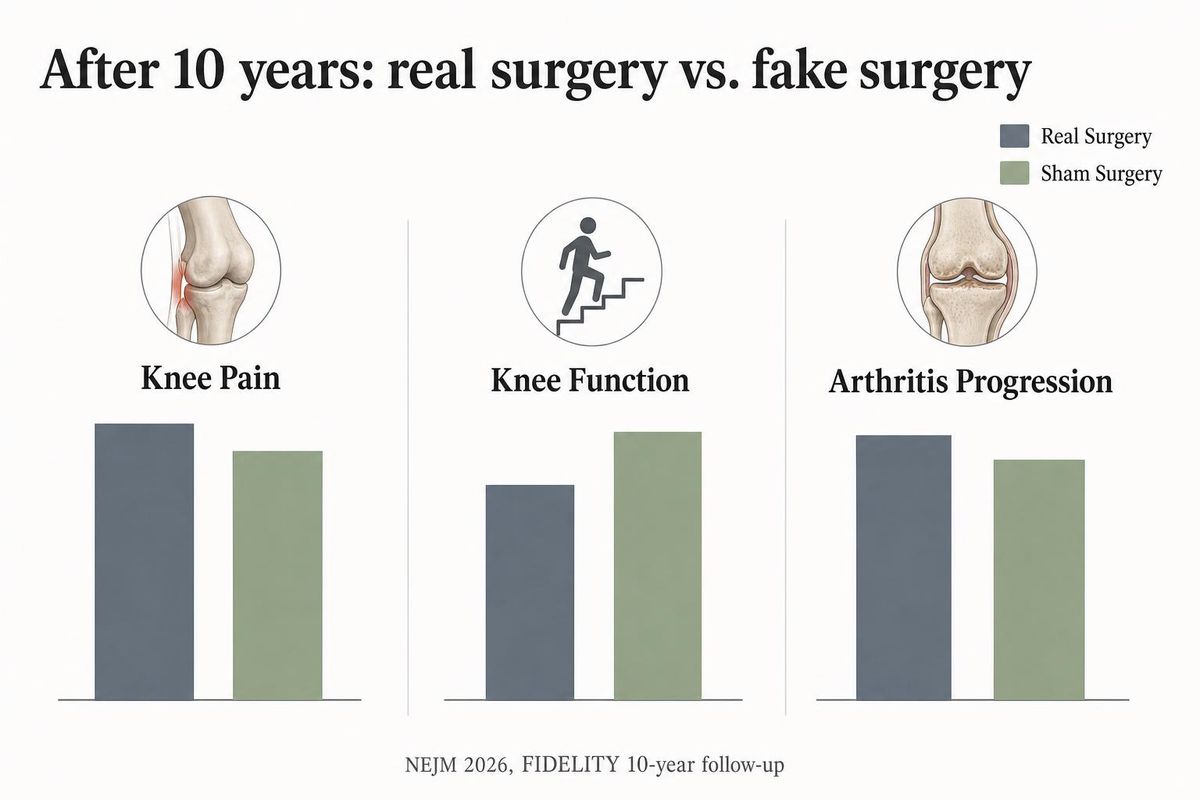
In May 2026, the New England Journal of Medicine published the 10-year follow-up of a trial out of the University of Helsinki. Here’s what makes it unusual: it had a fake-surgery control group. Half the patients got the real scope. The other half got cut, looked at, and stitched up. Same room, same anesthesia, same scar. Nobody knew which was which — not the patient, not the follow-up doctor.
At 10 years, the real-surgery group had more knee pain, worse function, and faster arthritis than the fake-surgery group. They were also more likely to need another knee operation later. Not “no better.” Worse.
The lead investigator, Dr. Teppo Järvinen, didn’t soften it: “For the procedure to be considered viable, one would expect some indication or proof of benefit, not quite a consistent proof of harm.” A Finnish surgeon, in a top journal, calling the standard fix for the most common knee diagnosis in adults a wash at best.
The US does about 205,000 of these surgeries a year. Roughly 95% are removals — trimming the damaged piece out — not repairs. That’s the procedure the 10-year data just torched.
“Degenerative” vs. “torn it skiing”
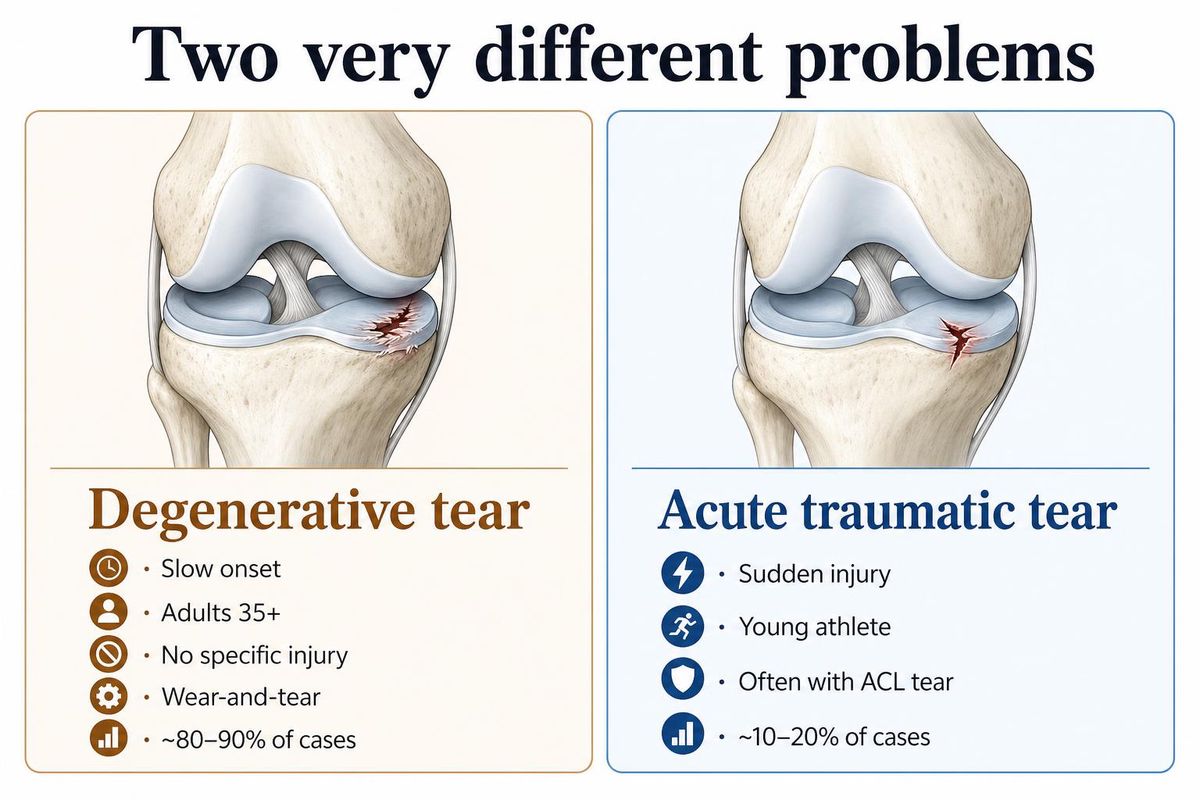
Before you panic and cancel something, here’s the most important distinction in this whole conversation.
Degenerative tears. Adults 35 and up. Slow onset. No specific injury. Your knee just started bothering you. You got an MRI, the report said “horizontal cleavage tear” or “complex degenerative tear.” This is the wear-and-tear category. About half of healthy 50-year-olds with no knee pain have one of these tears on MRI — they just don’t know it. Nobody scanned them. This is the category the new study covered. This is the category where surgery doesn’t help.
Acute traumatic tears. Young athlete, sudden injury, often a twist with a planted foot. Often comes with an ACL tear too. Different problem. The 2024 AAOS clinical guideline is clear: for these tears, repair (sewing the meniscus back together) beats removal. Done within three weeks, the repair holds up better long-term.
If you’re 28 and you blew your knee out in a soccer game last month, this post isn’t really about you. Go see a surgeon who does a lot of repairs, not removals. If you’re 42, you don’t remember hurting it, and your MRI reads like Latin — keep reading.
The thing that does work

So if scoping a degenerative meniscus tear doesn’t help, what does?
Movement.
In April 2026, ScienceDaily covered a BMJ review by Yan and colleagues — 217 trials, 15,684 patients, decades of data. They were comparing kinds of exercise for knee arthritis. The winner, by a clear margin, was the most boring option in the room: aerobic exercise. Walking. Cycling. Swimming.
Not special rehab. Not yoga. Not the latest band-and-stretch routine. Just steady, moderate aerobic movement.
This study did not directly compare exercise to surgery — honest caveat. But layer it on top of the new 10-year sham-surgery data and the picture sharpens fast. Fake surgery beat real surgery at 10 years. Aerobic exercise beats every other conservative option we’ve measured. The cheapest, most available, least scary option has the best evidence.
Why does it work? The boring answer is also the right one: bloodflow. A joint that moves gets fed. A joint that sits still doesn’t. The cartilage that lines your knee has no blood vessels of its own — it gets its nutrition from the fluid that gets squeezed in and out of the joint when you move. Walk, bike, swim, and the knee gets fed. Sit, and it doesn’t.
Dr. Howard Luks, a sports-medicine surgeon who’s been writing about this for years, puts it this way : “Most people with degenerative meniscus tears may have one or two exacerbations or periods during the year where their knee hurts — but, by and large, they get around just fine and lead very active lifestyles with these degenerative tears and do not require surgery for treatment of those tears.”
In other words: the knee will flare up sometimes. You’ll have a bad week. Then it’ll be fine again. That’s normal. That’s not a surgical problem.
The cost of the wrong choice

Even setting aside whether it works, scope surgery isn’t free.
Uninsured, meniscus surgery runs $5,000 to $15,000 for a simple case, up to $30,000 for a hard one. With insurance, you’re typically looking at $500 to $5,000 out of pocket. And for patients under 50 who get this surgery , about 1 in 25 end up needing a full knee replacement within seven years. Not a coin flip. But not nothing — especially if you’re 40 and you’d like to still be hiking at 65.
You also lose 6 to 8 weeks to recovery, and 3 to 6 months before you’re back to full sport. Conservative rehab — walking, biking, swimming, building the muscles around the joint — gets most people to full activity in 6 to 12 weeks. No scar, no anesthesia, no risk of a second surgery later.
Worth thinking about before the OR gets penciled in.
When surgery is genuinely the right call

I’m not anti-surgery. I had it. Some people need it. The honest list comes down to one word: bloodflow.
The meniscus has two zones. The outer rim — the “red-red zone” — is fed by blood vessels. Tears there can heal. The inner part has no blood vessels at all. Tears there can’t heal, no matter how much rehab you do. That’s the difference between a knee that fixes itself and a knee that needs a surgeon.
Your knee is locked. You can’t straighten it. A piece of cartilage is flipped into the joint and won’t reduce. Sometimes a manual move — what a doctor, or two training partners in the morning class, can do — pops it back. If that doesn’t work, or it keeps locking up, that’s surgery. That was me. My tear was in the avascular zone — no blood supply, getting worse, not going to heal on its own. The manual reductions worked in the moment, but the tear was never going to close. Eventually you stop fighting that.
You’re young, you blew it out in a real accident, and the tear is in the well-supplied outer zone. Get a surgeon who repairs rather than removes. The 2024 AAOS guideline is clear that saving the meniscus beats trimming it out — long-term arthritis risk drops a lot when the tissue stays in the joint.
A bucket-handle tear in the peripheral, well-supplied zone. These heal well with stitches. Even with a delay , a planned repair holds up.
That’s roughly 10 to 20% of meniscus cases. Not 100%. The other 80 to 90% — adults with slow, age-related wear after 35 — do best on the rehab path, not the OR.
If you want to think about this more broadly, we wrote a piece on how exercise stacks up against meds for depression , and another on the new brain-aging research and what protects against it. Same theme across all three: the cheap, available, scary-feeling option keeps quietly winning in trials.
So where does grappling fit
I run a Brazilian Jiu-Jitsu academy in Madison, so I want to be honest about how the mat fits into a knee story.
BJJ is a dynamic art. You’re loading the knee in dozens of directions over the course of a class — bending, rotating, posting, sweeping, recovering. That kind of varied, controlled loading is the opposite of how most adults treat their knees, which is mostly straight-line walking and a lot of sitting. Done right, it sends bloodflow through the joint, builds the muscles around it, and trains the knee to handle real-world positions with confidence.
“Done right” is the part I take seriously. We run a technique-first format. The high-risk knee submissions get trained progressively, not handed to brand-new white belts in their first roll. New adults get partnered with people who train safely. And I actively coach to it on the mat. If I see two athletes mid-roll setting up a position where someone’s knee is about to load badly, I stop the action and walk them through what to do instead. That’s the job. A coach who watches the mat catches a hundred small things a week that a self-guided gym workout doesn’t.
The mat is also one of the few places adults regularly practice managing pain that comes and goes — without freezing up, without panicking, without quitting. If your knee says “not today,” you sit out a round. We have plenty of members in their 40s and 50s working around old injuries — including people who came to BJJ to rebuild what stopped working in their 30s. Your first month is built around getting comfortable with that, not getting wrecked.
It’s not the right move for everyone with a knee history. It’s a good move for some — usually after a few months of walking, cycling, swimming, and a green light from a physical therapist who knows what BJJ actually involves.
If you have a knee story
If you’ve got an MRI report sitting in your inbox, a scar from a previous scope, or a friend who just got handed an OR date — come talk to a coach.
We do a 30-minute, no-class, no-pressure meeting. You tell us what your knee has been through. We tell you honestly whether the mat is a fit, when it’s a fit, and what we’d want you to do first. Sometimes the answer is “yes, come try a class.” Sometimes it’s “walk for three months, then we’ll talk.” It’s free, you don’t have to work out, and you’ll leave knowing more about your knee than you did walking in.
Book a free meet-the-coach session. 30 minutes, your story, our honest read. We’re at 3214 Kingsley Way on Madison’s west side, and we’ve been doing this since 2018.
Whatever you decide, the research is on the side of moving. Don’t let a scary MRI report stop you from walking.
- Knee health
- Movement is medicine
- Bjj madison
Ready to Start Your Journey?
Choose the option that works best for you
Call to book: +1 (608) 416-1140